Total Parenteral Nutrition (TPN) in home health involves the administration of a complete, intravenous (IV) solution of nutrients directly into a patient's bloodstream when they are unable to eat or absorb food through the digestive tract. This type of nutrition is typically provided for patients with severe malnutrition or medical conditions that impair digestion or absorption, such as certain cancers, gastrointestinal diseases, or complications from surgery.
TPN is designed to provide all the necessary nutrients that the body requires, including:
Key Components of TPN in Home Health:
1. Assessment and Preparation
- Patient Assessment: A comprehensive evaluation of the patient’s nutritional needs, medical condition, and ability to tolerate TPN is conducted. This includes reviewing lab results (e.g., blood work, electrolytes) to determine what nutrients are needed.
- Customizing the TPN Formula: Based on the patient's condition and nutritional requirements, healthcare providers (typically doctors and dietitians) prescribe a customized TPN formula to meet the patient's exact needs.
- Choosing an Access Site: TPN is administered through a central venous catheter (CVC) or peripherally inserted central catheter (PICC), which is placed into a large vein (usually in the chest or upper arm). These access points are selected because they can handle the high osmolality of the TPN solution and provide consistent, long-term access.
2. TPN Administration
- Infusion Process: The prescribed TPN solution is infused into the bloodstream over a specific period of time, typically over 12-24 hours, depending on the patient's needs and the type of solution being used. This is usually done overnight, allowing the patient to receive nutrients continuously while they sleep.
- IV Pump or Gravity Drip: The nurse uses either an IV pump or gravity drip to administer the TPN solution. The pump is more common for precise control over the infusion rate.
- Monitoring During Infusion: Nurses monitor the patient for any signs of complications, such as infection at the catheter site, changes in vital signs, or fluid imbalances.
3. Monitoring and Adjustments
- Regular Monitoring: Nurses monitor the patient’s response to TPN therapy, including checking vital signs, blood glucose levels, and laboratory values (e.g., electrolytes, liver function, kidney function) to ensure proper nutrition and hydration.
- Adjustments to TPN Formula: Based on laboratory results and ongoing assessments, the TPN formula may be adjusted to better meet the patient’s nutritional needs or to address any imbalances in nutrients or electrolytes.
- Complication Monitoring Nurses closely watch for complications like infections (at the catheter site or systemic), liver dysfunction, blood clots, electrolyte imbalances, and hyperglycemia (high blood sugar).
4. Patient and Caregiver Education
- Catheter Care: Nurses educate the patient and caregivers on how to care for the central venous catheter or PICC line, including cleaning the insertion site, monitoring for signs of infection (e.g., redness, swelling, fever), and proper techniques for line maintenance.
- TPN Administration: Patients and caregivers are trained on how to prepare and administer TPN if the patient is capable of doing so. This includes understanding how to handle the TPN bag, ensuring sterile techniques to avoid infection, and knowing how to monitor for any signs of adverse reactions during the infusion.
- Recognizing Complications: Nurses educate the patient and caregivers about signs of potential complications, including fever, chills, difficulty breathing, changes in mental status, and any signs of infection, and when to contact the healthcare provider.
5. Nutritional Support and Adjustments
- Regular Nutritional Evaluation: Dietitians or ealthcare providers reassess the patient's nutritional needs regularly based on ongoing medical conditions, lab results, and overall health status.
- Transitioning to Oral or Enteral Nutrition: As the patient’s condition improves and if they are able to tolerate oral or enteral feeding (through a feeding tube), the healthcare team may gradually reduce the TPN infusion or transition them away from TPN.
6. Risk Management and Complications
- Infections: Because TPN is delivered through a catheter directly into the bloodstream, there is a significant risk of infection, either locally at the catheter site or systemically. Nurses use sterile techniques during catheter maintenance and educate the patient and caregivers on preventing infections.
- Metabolic Complications: Patients on TPN are monitored closely for metabolic disturbances, such as hyperglycemia, electrolyte imbalances, or liver dysfunction, which can arise due to the nutrient composition or the prolonged use of TPN.
- Liver Disease: Long-term use of TPN can sometimes lead to liver complications, so liver function tests are regularly performed to monitor the patient's condition.
- Blood Clots: There is a risk of developing blood clots in the catheter (catheterrelated thrombosis), which requires monitoring and possibly treatment to prevent further complications.
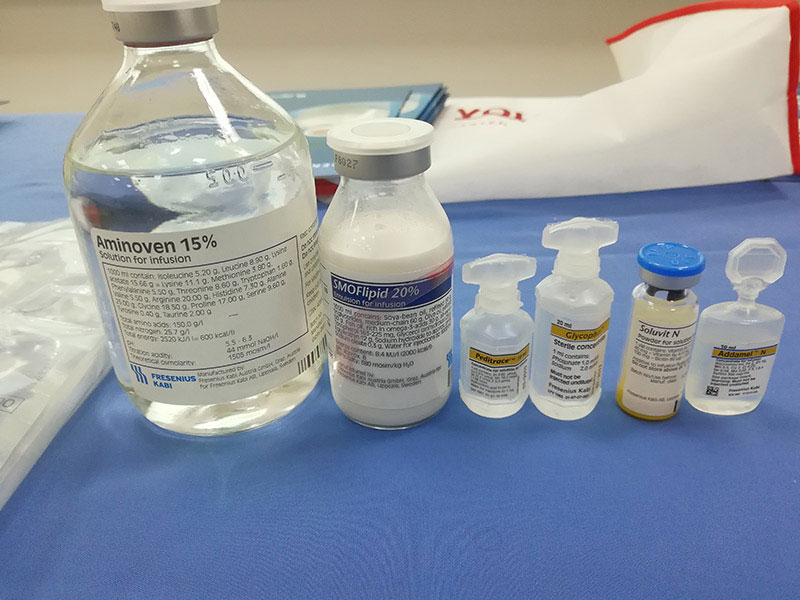 Ashashyou / Wikimedia Commons / CC BY-SA 3.0
Ashashyou / Wikimedia Commons / CC BY-SA 3.0
Benefits of TPN in Home Health:
- Convenience and Comfort: TPN allows patients to receive life-saving nutrition in the comfort of their home, reducing the need for hospital stays or frequent clinic visits.
- Improved Quality of Life: It helps patients maintain proper nutrition and prevent malnutrition, improving their overall health and ability to recover from medical conditions or surgeries.
- Cost-Effective: Home-based TPN can be more affordable than inpatient hospital care, reducing hospital readmission rates and providing care at a lower cost.
Risks and Challenges:
- Infection: The most common and serious risk of TPN is infection at the catheter insertion site or in the bloodstream (sepsis). Strict hygiene practices and regular monitoring are required to prevent this.
- Metabolic Imbalances: Patients may develop issues with blood sugar control, liver function, or electrolyte levels.
- Long-Term Dependency: Some patients may need TPN for extended periods, potentially causing complications like liver damage or difficulty transitioning back to oral feeding.
In Summary:
Total Parenteral Nutrition (TPN) in home health provides essential nutrition to patients who cannot consume food orally or absorb nutrients through the digestive system. Administered intravenously, TPN is tailored to meet the individual patient’s nutritional needs and can help improve their overall health and quality of life. Home health nurses play a crucial role in administering, monitoring, and adjusting TPN, while also providing education on safe catheter care and recognizing potential complications. Though TPN offers significant benefits in terms of comfort and convenience, it requires careful monitoring and management to prevent complications such as infections and metabolic disturbances.