Pain management in home health focuses on providing relief from pain and improving the quality of life for patients receiving care at home. This can include both acute pain (due to surgery, injury, or illness) and chronic pain (such as from arthritis, cancer, or other long-term conditions). Home health providers, particularly nurses, physicians, and other healthcare professionals, work with the patient to develop personalized pain management plans.
Key Components of Pain Management in Home Health:
 Belbury / Wikimedia Commons / CC BY-SA 4.0
Belbury / Wikimedia Commons / CC BY-SA 4.0
1. Pain Assessment
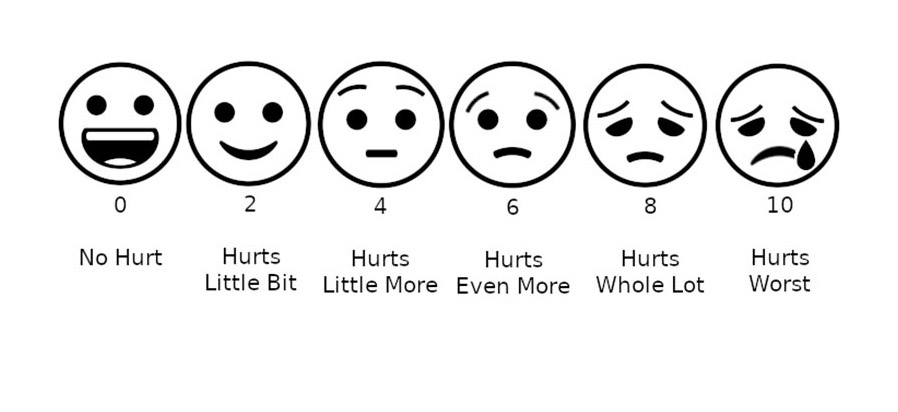
- Comprehensive Evaluation: Pain management begins with a thorough assessment of the patient’s pain. Healthcare providers ask the patient to describe the type, intensity, location, duration, and frequency of pain. Common pain scales (such as the 0-10 Numeric Rating Scale or the Wong-Baker FACES Pain Scale) are used to measure pain intensity.
- Identifying Underlying Causes: Understanding the source of the pain is essential for effective management. Whether the pain is from an injury, surgery, infection, or chronic illness, the healthcare team identifies the root cause to guide treatment.
2. Medication Management
- Pharmacological Options: Medications are a core component of pain management. These may include:
- Nonsteroidal Anti-inflammatory Drugs (NSAIDs): Used for mild to moderate pain (e.g., ibuprofen, acetaminophen).
- Opioids: Stronger painkillers for moderate to severe pain (e.g., morphine, oxycodone, hydrocodone). These are often prescribed for cancer pain, post-surgical recovery, or severe injuries. Opioids must be carefully managed due to the risk of addiction and side effects.
- Adjuvant Medications: Drugs that may not be primarily used for pain but can be effective in managing specific pain types (e.g., antidepressants for nerve pain or anticonvulsants for neuropathy).
- Topical Treatments: Topical creams or patches (e.g., lidocaine patches, capsaicin cream) can be applied directly to painful areas to provide localized relief.
- Patient and Caregiver Education: Home health professionals educate patients and caregivers about proper medication use, dosages, potential side effects, and safety, especially for opioid medications.
3. Non-Pharmacological Pain Management Techniques
- Physical Therapy: A physical therapist may work with the patient on exercises or movements that reduce pain, improve strength, and increase mobility. Techniques like stretching, strengthening, and postural adjustments can relieve musculoskeletal pain.
- Hot/Cold Therapy: Applying heat or cold packs can help reduce inflammation, ease muscle tension, and promote relaxation. Ice may be used for acute injuries (e.g., sprains), while heat is often used for chronic conditions (e.g., arthritis).
- Massage Therapy: Therapeutic massage can help relieve tension and pain in muscles and soft tissues.
- Transcutaneous Electrical Nerve Stimulation (TENS): TENS units use lowvoltage electrical currents to relieve pain by stimulating nerves, which can block pain signals and improve circulation.
- Relaxation Techniques: Methods like deep breathing, guided imagery, and mindfulness meditation can reduce pain perception and help manage stress or anxiety that may contribute to pain.
- Cognitive Behavioral Therapy (CBT): CBT and other psychological interventions can be used to help patients change the way they think about and respond to pain, improving emotional and psychological well-being.
4. Patient and Caregiver Education
- Pain Management Plan: Home health providers work with the patient and their caregivers to create a tailored pain management plan that includes medication, lifestyle changes, and coping strategies.
- Managing Side Effects: Nurses educate the patient and their family about managing any side effects from pain medications (such as nausea, constipation, or sedation) and how to mitigate them.
- Setting Realistic Goals: Educating patients on setting achievable goals for pain relief helps them understand that complete elimination of pain may not always be possible but that improving comfort and quality of life is the primary goal.
- Signs of Complications:: Patients are taught to recognize warning signs of complications from medication, such as signs of overdose or adverse reactions (e.g., difficulty breathing or confusion with opioids).
5. Monitoring and Follow-up
- Regular Pain Assessments: Ongoing evaluation of pain levels is essential. Nurses or healthcare professionals continue to assess the effectiveness of the pain management plan and make adjustments as needed. This includes tracking changes in pain intensity, patient responses to medications, and whether side effects or complications arise.
- Medication Adjustments: If the prescribed pain management is not providing sufficient relief or if side effects occur, the healthcare provider may adjust the medication regimen or explore other options.
6. Coordination with Healthcare Providers
- Collaboration: Home health nurses and healthcare providers work together to monitor the patient’s condition and adjust pain management strategies. This may involve communication with primary care physicians, specialists (such as pain management doctors), and pharmacists to ensure that the pain management plan is optimized.
- Palliative and Hospice Care: For patients with serious, life-limiting illnesses, palliative or hospice care may provide more specialized pain management, focusing on comfort and quality of life rather than curative treatments.
 Toralf Thomassen / Unsplash
Toralf Thomassen / Unsplash
Benefits of Pain Management in Home Health:
- Improved Comfort and Quality of Life: Effective pain management helps patients feel more comfortable, improves their ability to engage in daily activities, and enhances overall well-being.
- Reduced Hospitalizations: Proper pain management at home can prevent the need for hospital visits, reducing healthcare costs and preventing unnecessary hospital admissions.
- Personalized Care: Pain management is tailored to the specific needs of the patient, allowing for individualized approaches that address both physical and emotional aspects of pain.
- Independence and Autonomy: Patients who receive pain management at home can maintain a high.
 Kampus Production / Pexels
Kampus Production / Pexels
Common Pain Conditions Managed in Home Health:
- Post-Surgical Pain: Pain following surgery, such as joint replacements, abdominal surgeries, or soft tissue repairs.
- MetCancer Pain: Pain from tumors, treatments like chemotherapy or radiation, or related complications.
- Arthritis and Musculoskeletal Pain: Chronic pain conditions, such as osteoarthritis or rheumatoid arthritis, can be managed with a combination of medication and physical therapy.
- Neuropathic Pain: Pain from nerve damage (e.g., diabetic neuropathy, shingles), often requiring specialized medications.
- Back Pain: Chronic back pain, often managed with a mix of medications, physical therapy, and pain management techniques.
- Wound Pain: Pain from chronic wounds, burns, or pressure ulcers, which requires careful management to ensure comfort during healing.
In Summary:
Pain management in home health is a critical part of caring for patients who suffer from both acute and chronic pain. It involves a combination of medication, non-pharmacological interventions (like physical therapy, hot/cold therapy, and relaxation techniques), patient education, and close monitoring. Home health professionals work closely with patients and caregivers to create personalized pain management plans that aim to improve comfort, reduce the impact of pain on daily life, and prevent complications. Effective pain management helps patients maintain a better quality of life while managing both physical and emotional aspects of pain.