Incontinence care in home health refers to the management and support provided to patients experiencing urinary or fecal incontinence while they are in the comfort of their home. Incontinence can significantly impact a person’s quality of life, causing emotional distress, skin issues, and social isolation. Home health services play an essential role in helping patients maintain dignity and manage their condition effectively.
Key Components of Incontinence Care in Home Health:
1. Assessment and Monitoring
- Identifying the Type and Cause of Incontinence: A thorough assessment is conducted by a nurse or healthcare provider to identify the type of incontinence (e.g., urinary incontinence, fecal incontinence, mixed incontinence) and its underlying causes (e.g., age-related changes, neurological conditions, prostate issues, or weakened pelvic muscles).
- Assessing the Severity: The healthcare provider will assess how severe the incontinence is, how often it occurs, and how it affects the patient's daily life. This helps guide the treatment plan and identify necessary interventions.
- Monitoring Skin Integrity: Incontinence can lead to skin irritation or pressure ulcers if not properly managed. Caregivers will monitor the skin for signs of redness, sores, or infection, especially in areas where moisture is present.
2. Personal Hygiene and Skin Care
- Routine Cleaning: Patients with incontinence need assistance with routine cleaning and changing to prevent skin irritation or infection. The home health provider will assist the patient in maintaining good hygiene, cleaning the affected areas gently, and ensuring that skin is kept dry.
- Skin Protection: Using barrier creams or ointments can help protect the skin from moisture and prevent breakdown. Healthcare providers will ensure that the skin is properly protected, especially for patients who have prolonged exposure to moisture.
- Frequent Monitoring and Changing: For patients with urinary or fecal incontinence, frequent changing of absorbent products, such as adult diapers or pads, is essential to avoid discomfort and prevent skin problems.
3. Use of Incontinence Products
- Absorbent Pads and Adult Diapers: Home health providers help select the right incontinence products, such as adult diapers, pads, or absorbent undergarments, that are comfortable and offer sufficient protection. They also guide the patient and family on how to use and dispose of these products properly.
- Catheters: For some patients, a catheter (either indwelling or intermittent) may be used to manage urinary incontinence. Home health professionals will assist with catheter care, including how to clean and maintain the catheter to prevent infections.
- Fecal Incontinence Management: For patients with fecal incontinence, there may be specific products like anal plugs or fecal management systems. The healthcare team will work with the patient and caregivers to ensure proper use and comfort.
 PatriciaMoraleda / Pixabay
PatriciaMoraleda / Pixabay
4. Bladder and Bowel Training Programs
- Scheduled Toileting: One of the primary strategies for managing incontinence is scheduled toileting or "timed voiding." This involves setting regular intervals for the patient to try to use the bathroom, preventing accidents by anticipating their needs.
- Pelvic Floor Exercises: For patients with urinary incontinence due to weak pelvic floor muscles, healthcare providers may teach exercises such as Kegel exercises to help strengthen these muscles, improving bladder control.
- Bowel Training: For patients with fecal incontinence, bowel training may involve strategies like timed bowel movements, dietary changes, and medications to help the patient develop a regular pattern of bowel movements.
5. Dietary and Fluid Management
- Fluid Intake Management: Managing the amount and timing of fluid intake can help patients with urinary incontinence. For example, avoiding large quantities of fluids before bedtime can reduce nighttime incontinence. Conversely, some patients may be encouraged to drink more fluids to avoid dehydration, which can worsen incontinence.
- Dietary Adjustments: Certain foods and drinks, such as caffeine, alcohol, and spicy foods, can irritate the bladder. Dietary adjustments may be recommended to avoid foods that exacerbate incontinence.
- Constipation Management: Constipation can contribute to fecal incontinence. A high-fiber diet, adequate fluid intake, and possibly mild stool softeners can help prevent constipation and manage bowel incontinence.
6. Medication and Treatment Options
- Medications for Urinary Incontinence: There are medications available for managing urinary incontinence, such as anticholinergics or beta-3 agonists. These medications help reduce bladder spasms, control urgency, and improve bladder capacity.
- Medications for Bowel Incontinence: Medications to control bowel movements may include anti-diarrheal medications or stool softeners, depending on the underlying cause of fecal incontinence.
- Topical Treatments: For patients with skin irritation from incontinence, topical treatments such as barrier creams, zinc oxide, or prescription ointments may be recommended to protect the skin and promote healing.
7. Physical Therapy
- Pelvic Floor Rehabilitation: For patients with urinary incontinence, especially those with weakened pelvic floor muscles, physical therapy (e.g., pelvic floor exercises) may be suggested. A trained physical therapist can work with the patient to improve muscle strength, coordination, and bladder control.
- Biofeedback: Biofeedback is sometimes used to help patients gain control over their pelvic floor muscles and improve incontinence symptoms. The therapist uses sensors to monitor muscle contractions, providing real-time feedback to help the patient strengthen the muscles that control urinary or bowel function.
 chormail153750 / Vecteezy
chormail153750 / Vecteezy
8. Assistive Devices
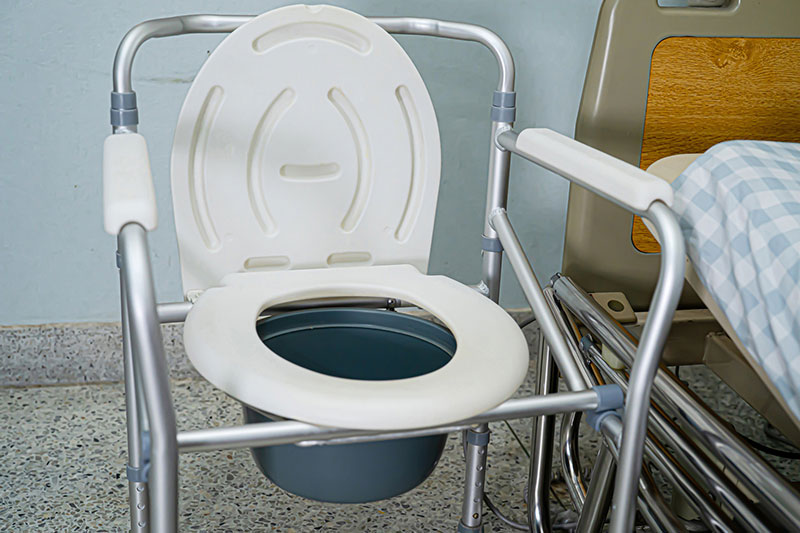
- Toilet Aids: For patients who have difficulty getting to the bathroom on their own, home health providers may recommend assistive devices such as raised toilet seats, grab bars, or bedside commodes to increase independence and reduce the risk of accidents.
- Urinals and Bedpans: For bedridden patients, urinals or bedpans may be used as a temporary solution to manage urinary or fecal incontinence, with proper cleaning and care to ensure comfort and hygiene.
9. Psychosocial Support
- Building Confidence: Incontinence can be an emotionally distressing condition, leading to embarrassment or social withdrawal. Home health professionals provide emotional support, encourage open communication, and work to minimize the stigma associated with incontinence.
- Family and Caregiver Training: Educating family members and caregivers about incontinence care helps them provide better support. This includes learning proper hygiene techniques, understanding incontinence products, and managing the emotional challenges that come with caregiving.
10. Education for Patients and Caregivers
- Self-Care Training: Home health professionals teach patients and caregivers how to manage incontinence independently and confidently. This includes proper hygiene, product selection, and when to seek medical help if symptoms worsen.
- Lifestyle Modifications: Patients and families are educated on lifestyle changes that can help improve incontinence, such as avoiding bladder irritants (e.g., caffeine), staying hydrated, and performing pelvic floor exercises.
 Giorgio Trovato / Unsplash
Giorgio Trovato / Unsplash
Benefits of Incontinence Care in Home Health:
- Improved Quality of Life: Effective management of incontinence can significantly enhance the patient’s quality of life, reducing discomfort, skin irritation, and the emotional distress associated with incontinence.
- Enhanced Dignity and Comfort: With the right support, patients can maintain their dignity, remain socially active, and continue daily activities with confidence.
- Reduced Risk of Complications: Proper skin care, hygiene, and use of incontinence products help prevent complications such as skin breakdown, infections, and urinary tract infections (UTIs).
- Independence and Empowerment: Education and training empower patients and caregivers to manage incontinence, enhancing their independence and self-confidence.
Challenges:
- Emotional Distress: Many patients feel embarrassed or isolated because of their incontinence, and addressing this emotional burden requires patience and sensitive communication.
- Caregiver Burden: Caregivers may experience physical and emotional strain when helping with incontinence care, so support and training are crucial.
- Cost of Supplies: Ongoing costs for incontinence products and medications can add up, and finding affordable options may be a concern for some families.
In Summary:
Incontinence care in home health focuses on improving the quality of life for patients dealing with urinary or fecal incontinence. By providing personalized support, including hygiene assistance, the use of appropriate incontinence products, skin care, pelvic floor exercises, and medications, home health professionals help manage this condition effectively. Education and training for both the patient and caregivers ensure that the patient maintains dignity and independence while preventing complications and improving comfort.